Tragic overdose deaths get media attention, but much of the harm is more ordinary and preventable. It includes suffering caused by ill-timed, unsought pregnancies that leave thousands of mothers and newborns struggling with opioid withdrawal together.
The scale of North America’s epidemic of heroin, oxy, and other opioids is staggering. Some 2.5 million people in the United States live with addiction or related drug problems that together are called opioid use disorder. The total costs to society may be as high as $500 billion annually.
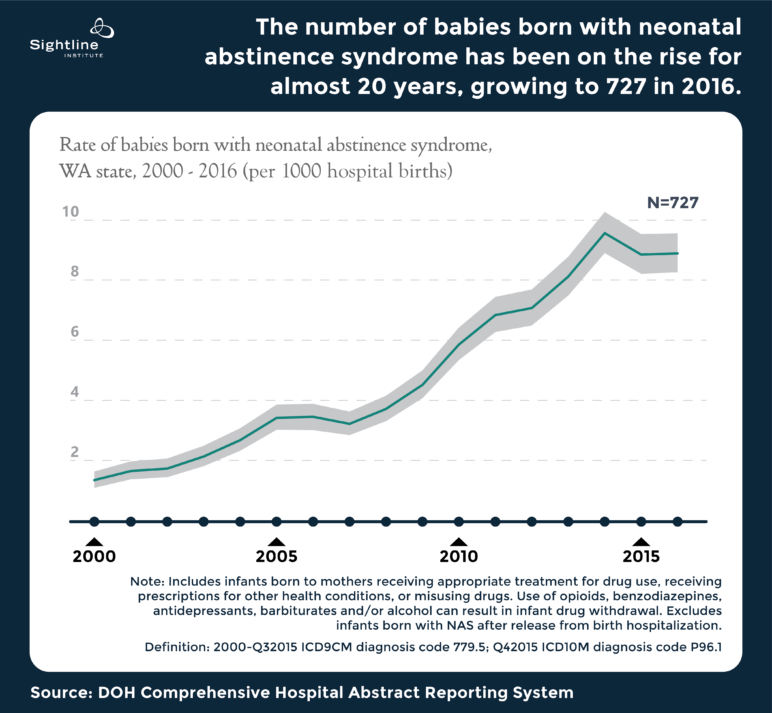
Tragic overdose deaths get media attention, but much of the harm is more ordinary and preventable. It includes suffering caused by ill-timed, unsought pregnancies that leave thousands of mothers and newborns struggling with opioid withdrawal together. Almost 1 percent of babies born in Washington State, for example, go through withdrawal from heroin and other opioids as soon as they’re born, as shown in the figure below. Of all the psycho-social and health problems that could be addressed during opioid treatment, few promise anything close to the potential cascade of benefits that come from empowering women, as they desire, to time their pregnancies and give their children the best possible starts in life.
Women with opioid use disorder (OUD) often find themselves dependent, impoverished or homeless—situations that put them at risk for sexual assault and exploitation and unable to find consistent, supportive reproductive care. Many would prefer to postpone pregnancy or to devote their energy to kids they already have. Eighty to ninety percent report that their pregnancies are unintended, and yet they use contraceptives at a lower rate than average and rely on less effective methods when they do.
Syringe exchanges and opioid treatment programs bring these women into contact with healers and social service providers and, therefore, create opportunities to offer family planning and other reproductive health services to women who want them. But, today, services for people with substance use disorders rarely include family planning or even screening for pregnancy desires. Better integrated care could change the lives of women with OUD and their families.
As British Columbia, Oregon, and Washington scale up opioid treatment services, they have an opportunity to show how that integrated care could work. The benefits are clear, especially as you take into account the difficult path for pregnant women dealing with OUD.
Hard Starts
When a woman dealing with substance use disorder finds herself unexpectedly pregnant, she faces a tough choice: she can terminate the pregnancy or carry it forward, and the goal of care is to create the best possible set of outcomes for mother and child either way. Trying to stop opioid use once pregnant is risky for mother and fetus, so when possible, women switch to methadone or a similar medication. But that brings its own set of challenges.
In the United States, over 20,000 babies come into the world each year addicted to opioids and promptly go into withdrawal. In Washington alone, the number had grown to 727 by 2016—0.8 percent of the state’s births that year (see figure below). These infants have what medical professionals call neonatal abstinence syndrome (NAS), which can be caused by untreated drug abuse or by a prescribed medication like methadone. NAS symptoms include tremors, fevers, spasms, breathing and feeding difficulties, and inconsolable distress. Many infants with NAS require extended hospitalization—on average for just over two weeks—so that medical professionals can manage their withdrawal symptoms by providing tapered doses of morphine.
We know that treatment with methadone or a similar medication is safer than a woman trying to stop using opioids altogether. Even so, nurses who work in neonatal care units say that the cries of infants going through withdrawal can be heartbreaking. Part of that anguish falls on mothers who never meant to impose such suffering on a child and who sometimes “room in,” a promising practice that promotes bonding and lets them be present throughout their babies’ hospitalizations. Switching from an opioid like heroin to a supervised medication like methadone during pregnancy is a positive step for a woman with OUD, but for those who aren’t yet pregnant and might desire to avoid pregnancy, we can do better.
Omissions and Opportunities
Pregnancy timing is fundamental to women’s health and mental health as well as the health of babies, which is why a growing number of healthcare providers now ask all women of reproductive age a simple screening question, Would you like to get pregnant in the next year? This inquiry is the heart of Oregon’s One Key Question Initiative. It has become a national model to identify women who could benefit from either contraception or pre-pregnancy preparations, or both.
But this simple screening question is not yet routine in medication-assisted treatment programs and other services for women with substance use disorders. Federal guidelines for such programs require screening for pregnancy itself and referral to prenatal care for women who are pregnant. (They also require screening and referral for an array of common health and mental health issues.) What they don’t require is the kind of screening and service referral that would help women to time or prevent pregnancies according to their preferences.
When asked, women in treatment have expressed interest in receiving family planning services at their treatment center. Truly comprehensive care would include access to abortion for women who want to terminate unsought pregnancies, non-judgmental prenatal care for women who want to continue their pregnancies, pre-conception care for women who are desiring pregnancy or unsure, and contraception for women wishing to avoid pregnancy.
Model Care at Seattle’s Syringe Exchange
Dr. Lauren Owens, a Family Planning Fellow, is exploring how best to offer low-barrier reproductive health services to women who use Seattle’s syringe exchange. The project was inspired in part by a program in Baltimore, where women receive contraceptives and other reproductive health services as part of a mobile needle exchange. Most Baltimore participants who wanted birth control opted for an injectable method, which is more reliable than pills or condoms.
Despite the need and desire for more accessible family planning services, patient-provider conversations need to put patient autonomy first, Owens says. In our society, addiction often is stigmatized instead of being viewed as substance use disorder, a medical issue. This is particularly true for women with substance use disorders, and even more so if they are pregnant. Consequently, many patients have had bad experiences with the medical system and avoid seeking reproductive health care because they expect shame and judgment.
Also, trauma is common among women with substance use disorders including opioids; 75% of clients in substance use treatment settings report a history of trauma. A history of sexual trauma is associated with avoidance of routine gynecologic care. Patient-centered care and shared decision-making are key to providing sensitive reproductive health care in this population. When providing care at the syringe exchange, Owens invites conversation about reproductive health; if a woman doesn’t want to discuss contraception, Pap smears, or STD testing, they stick to the patient’s agenda.
Scaling Up
There’s never been greater attention placed on opioid use disorders in terms of funding from federal, state and provincial agencies in Cascadia. British Columbia, the epicenter of Canada’s opioid crisis, declared a public health emergency in 2016 and created a Ministry of Health and Addictions. Modeled in part on Portugal’s decriminalization approach, the Ministry is focused on minimizing risks and harms linked to drug use.
Washington is rolling out regional opioid treatment services as part of the federal Medicaid Transformation process. This approach is implemented through nine regional “Accountable Communities of Health,” or ACHs for short. The ACH in Pierce County has already committed to integrate high-quality reproductive and maternal health into opioid treatment.
Pierce County ACH broadly encourages the One Key Question approach. “We’ve also added men to that approach,” says CEO Alisha Fehrenbacher. Women and men are asked about their parenthood desires, so that follow-up care can be based on their response.
A pilot project focuses on the special needs of pregnant women with opioid use disorder. Better care coordination for these women might include helping them attend medical appointments and get their prescriptions filled while addressing core issues vital to a person’s health, such as housing, transportation and food—and reproductive care as appropriate.
In the northwest corner of Washington, the North Sound ACH is actively exploring similar options. In 2017, it completed an “early wins” project that made state-of-the-art contraceptive devices—IUDs and Implants—more available to women who want them by training counselors and providers.
More Respect, Better Care
To ensure that health care is culturally humble and equitable, Pierce County ACH offers awareness and sensitivity education to providers. “This is especially critical when working with a person who is abusing substances. We must remove the stigma of substance abuse, so we may provide the most appropriate and effective care possible,” Fehrenbacher says.
Certified nurse midwife Katharine Harkins suggests that one way to reduce perceived judgement is to make questions about pregnancy desires a normal, universal part of medical care. “Health care professionals now routinely screen for depression and domestic violence, and people don’t feel singled out or judged, because everyone gets asked,” says Harkins. “It’s not ethical to identify these other conditions using universal screening but omit pregnancy timing and prevention. When we leave this out, women are missing out on essential medical information and opportunities to protect their health and the health of children they may choose to have.”
For women fighting OUD, an unexpected pregnancy or ill-timed birth can be an intense life stressor and may jeopardize recovery. When we fail to ask about this dimension of life and provide needed services, we miss opportunities to improve health and wellbeing. More significantly, women with substance use disorder, like all of us, deserve to plan their families: to have the children they want to have when they want to have them.

Sensitively written, including the info on trauma and addiction. By any chance, do you know the percentage of babies born affected by fetal alcohol? It would help put this information in context.